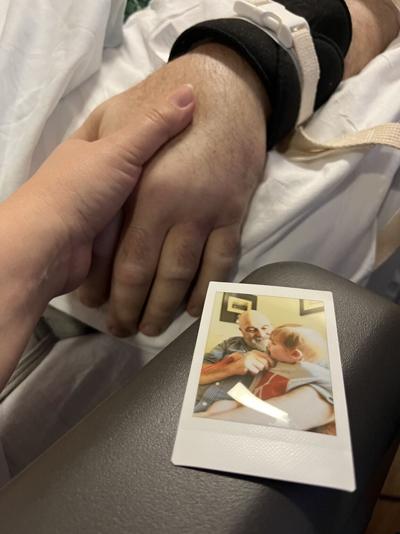
Cat Murphy holds her father's had while he is hospitalized with histoplasmosis.
In September and October, some Williamson County and Maury County residents fell ill with what they thought was the flu or another virus, only to later discover it was the fungal infection histoplasmosis.
Some of the first cases identified are still not out of the woods yet, patients tell Scene sister publication the Williamson Scene.
In early December, the Tennessee Department of Health issued a Health Alert Network advisory to alert clinicians to an increase in histoplasmosis cases in Williamson and Maury counties. In late January, the department had confirmed 36 cases, and early this month the case count had reached 40, the department confirms.
Cat Murphy's father was hospitalized from September through most of February due to the infection. Her father's illness has lingered longer than she anticipated, with the addition of a number of hospital-acquired infections and reinfections. It's a delicate balance to treat the infection while treating his existing autoimmune disease.
“It’s been a lot of three steps forward, two steps back,” Murphy says.
Murphy, a Middle Tennessee native, was often warned not to play in a bird bath as a child because of histoplasmosis, which stems from soil contaminated by bird or bat droppings and is endemic to the area. It was a boogeyman — a threat, she says.
“It was not the first thing on anybody's bingo card, for sure,” she says of her father's illness. “They were looking at flu and stress and COVID and tick-borne diseases and everything you could think of before we finally found out that this is what had been going on the whole time.”
Delay in identifying the infection is a theme among patients.
Kathy York started feeling sick in early November and chalked it up to a virus. But even after taking antibiotics, her fever didn’t subside. She set an appointment with an infectious disease expert, but that was weeks away, and they wouldn’t let her visit in person because of the fever she couldn’t shake.
After the health department notification came out, York's boss, a GI doctor in the area, offered her a test — a urine sample that she sent out to a lab.
“It needs to be tested for sooner than later,” York says. “If we know it's endemic here, why are we not testing people that come in with fever of an unknown origin?”
It was 25-year-old Liam O’Neal’s dermatologist who suggested the test, after he was first misdiagnosed with pneumonia. He immediately started medication after being diagnosed on Nov. 1, but in the days following, he had breathing trouble and suffered a seizure and pulmonary arrest followed by cardiac arrest. He needed resuscitation and was eventually put on a ventilator and ECMO. (His case has since garnered national attention).
O’Neal, a type 1 diabetic, spent November in intensive care, followed by two weeks of inpatient care, and two more weeks in the hospital because he couldn’t keep down food or liquids. He has lost 86 pounds, and racked up $2.4 million in hospital-stay bills, which is mostly covered by insurance, his mother Amy O’Neal says.
Before lawmakers gavel out this year — ahead of an election cycle — a bill designed to protect pesticide companies’ liability remains uncertain
Kidney and gall bladder issues remain today, and he must continue treatment until October. He has to walk with a walker, can no longer play hockey, and has missed out on work opportunities. Amy O’Neal lost her job because of all of the work she missed caring for her son.
“For us, had they tested him originally, we may not have ended up on life support and him struggling with everything that he struggles with now,” she says.
York is finally starting to feel better after the treatment regimen took her from feeling bad to worse. She had adverse reactions to the treatments (namely amphotericin B, a powerful antifungal medication reserved for life-threatening infections), including swelling in her legs and intense joint pain. After two weeks in the hospital to receive the medication intravenously, York is still using a heart monitor and has a stress test ahead. The medication made her so sick that she finished just two months of treatment rather than the recommended three, so she runs at least some risk of it coming back.
“It's not easy to get over,” she says. “I think everybody's still going, 'When are we going to feel good?' I was just unlucky. All of us just walked in the wrong area at the wrong time.”
York walked five miles every day, which included to the top of her subdivision, watching the progress of the widening of Buckner Lane, near June Lake Road. She wonders if there is negligence involved in soil testing before the construction, but suspects everyone has been too sick to even look into it.
Amy O’Neal is convinced the origin of the infection is the June Lake construction in Spring Hill too. In her own research, she has found that many of the cases are within a mile or two of each other.
“It's bad to point the finger, put the blame on somebody,” she says. “But could there have been something done to make it not as severe? I don’t think we’ll ever really know, but it would be nice.”
For now, Liam O'Neal's family is celebrating his 25th birthday, which is extra sweet this year after that scary patch in November.
Murphy’s Facebook group provides some solace as the patients begin to recover and search for causes.
“It's just nice to at least acknowledge that there are other people, that it’s not just us,” Murphy says. “I think we all just still really want to know how and why this happens to the people that we love.”
The Williamson Scene reached out to Southeast Ventures, the developer behind construction near June Lake Road, but received no response.
This article was first published by our sister publication, the Williamson Scene.